This post is part of a series about my brother’s upcoming book Addiction Nation: What the Opioid Crisis Reveals about Us, discussing some of the science and stats he used throughout the books. Read the intro post here, part 1 here, part 2 here, or (best of all) pre-order the book on Amazon here.
Okay, so last week you heard about how Tim had to change a few things around when we read the actual research. Today I wanted to talk about a few pieces of research that were included in the book that have some controversy around them. While there’s only so much you can fit in a book, we thought the blog might be a good place to expand a little on some of the studies quoted. How does that sound brother?
Tim: Perfect! This was another tricky area of wading through a lot of conflicting information. One thing that I don’t think your readers will be surprised by is that the reason some of these studies are controversial is not always about the studies themselves but the claims or coverage that comes out of them.
For example, the claim “environmental factors play a role in addiction” isn’t controversial. What is controversial is when a study is used, or it’s author claims, that they have demonstrated that environment is ALL or most of what matters.
My general standard was to imagine a reader diving into a specific study in more detail. As they read, would they feel like they were learning nuance and adding texture? Or would the feel like they were misled?
That sounds like a pretty reasonable standard to me! And yes, “blame the journalist” has been a catchphrase on this blog since the very beginning. Coverage of studies can certainly skew perception of the study in ways authors never intended.
Alright, first up, a study I’ve actually blogged about before “Rising morbidity and mortality in midlife among white non-Hispanic Americans in the 21st century“. Before we get to the meat of this, I gotta point out brother, you actually got the name of this study wrong in your citation list. You called it “Rising morbidity and mortality, US Whites”. I mean I know I’m the only one who’s gonna read through all your citations, but GET. IT. TOGETHER. Luckily for you the author, journal, year, and DOI number were all correct, so I’ll let this one slide.
Edited even before Tim could reply: I actually just figured out how this happened. On the study page I just linked to if you click “citation manager” it changes the name of the study to the one Tim used

I take it all back brother, you’re okay.
Tim: Oh dear readers… You have no idea how sweet this is. I tried to find an emoji for the feelings you feel when your sister who is always right isn’t right but I just couldn’t find one that could encapsulate how great I feel right now.
Okay, okay, simmer down here kiddo. I actually was right. The name of the paper you used in your citation list isn’t the one it was published under. I was just clarifying that your error wasn’t your fault.
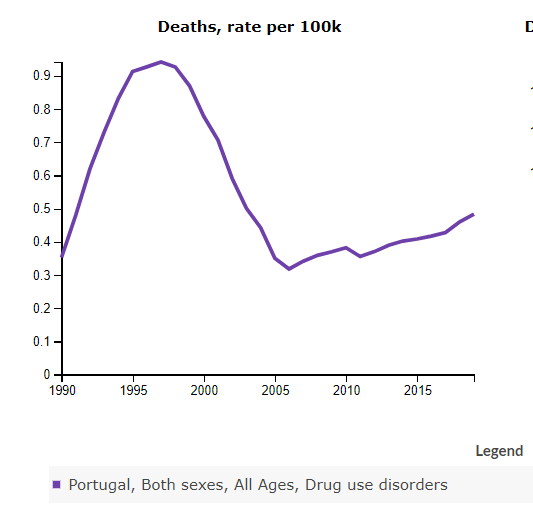
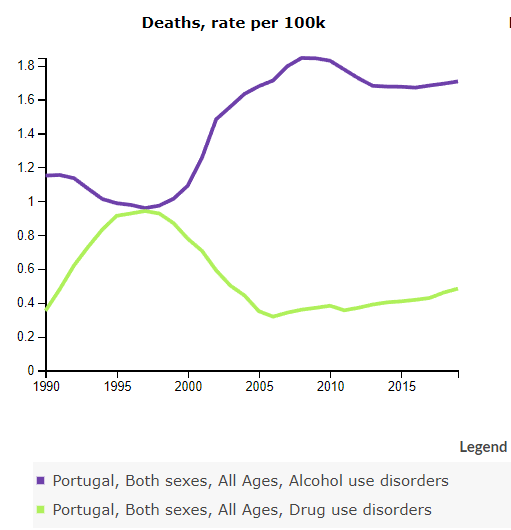
Anyway, your quote in the book about this study (Chapter 7) is this:
After decades of declining mortality rates – primarily because of gains in treating cancer and heart disease – the likelihood of a white person dying between the ages of forty-five and fifty four has gone up. A similar trend has not been seen in any of the world’s wealthiest nations……The change was driven was driven almost entirely by drug -and alcohol-related liver disease, and suicides.
You use the study above to support this quote, and you accurately state what the study concluded. However, there have been a few follow ups that I blogged about here.
First, Andrew Gelman questioned the findings of the initial study, citing cohort effects as possible confounders. Then, another study came out that suggested that the overdose increase was real, but not the suicide rate increase. Then in 2018 the CDC released a report that showed that suicide rates were at a 50-year peak. They didn’t specifically quantify based on race, but they did show that rural areas (which tend to be whiter) were more vulnerable.
There’s a lot going on here, but I think overall it seemed like a reasonable quote for you to leave in. I’d say one of the big challenges of editing a non-science book for scientific accuracy is how to explain things like this without derailing the whole book. The point of your chapter was supposed to be Despair and Acedia, not demographic trends. It seemed like the initial study got enough right that it was worth quoting, but I still feel like we’re refining the details. Personally, I would have put more of that in, but I know you had space limitations. Any thoughts on this?
Tim: More got cut from this book than made it in the final copy. Final word count is around 70,000 and I left 100,000 words on the cutting room floor. That isn’t just rewrites but all the sections and chapters that didn’t make the final cut. It is tough to figure out how much space you can dedicate to the nuances or follow ups of specific studies.
And with the specific details of which “deaths of despair” were most responsible, it gets pretty complicated. My guess is there will be some back and forth about this for a while because of how hard it is to feel confident in how deaths are categorized.
There is a real human somewhere who needs to go through and catalog cause of death. And, whether or not someone died by suicide or via an accidental overdose is a line that is not always clear. Social norms or even the kind of reporting forms used can influence how these numbers are counted.
We will also likely see studies in the future that see what sort of effects the high overdose rate will have on those who might have died later from alcohol-related health issues or by suicide. The main question there being whether or not these deaths are concentrating when in previous cohorts they would have spread more evenly over several decades.
The lines are blurry enough for me that I felt the overall point about “deaths of despair” stands even as researchers try to parse out in greater detail what is going on.
Alright, next up we have the infamous Rat Park study. From the work of Bruce Alexandar, this is one of the most quoted studies on addiction. Basically, the researchers put rats in empty cages with morphine and noted that the rats became addicted very quickly. They then put them in a nice environment and discovered that they rarely got addicted to morphine. This study is often used to prove that when it comes to addiction, environment matters more than exposure to drugs.
Now while I agree this study is interesting, I do have some concerns. Scott Alexander over at Slate Star Codex raised some issues with this study a few years ago with this post. He points out that while some studies have mostly replicated the effect, other studies have not. More than that though, the two things that seemed to most stand out where:
- Genetics studies that produce results like this:
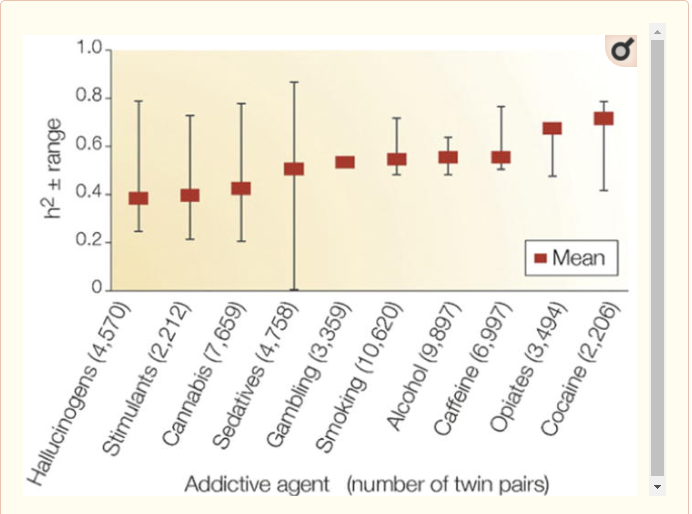
- The pretty observable fact that the rich and famous still have drug and alcohol problems. As the SSC post points out, Celebrity Rehab with Dr. Drew was canceled by the host after he said “he was tired of the criticism leveled at him after celebrities he treated had relapsed into addiction and died”. Given that celebrities have access to some of the nicest environments in the world, it seems hard to says it’s all about environment.
You nod to the controversy in the book with this note:
Alexander doesn’t deny that a wide range of other factors including genetics, life experience and individual choice plays a role, but he believes they need to be put into the background because of the power of the social forces at play.
That’s a good note, and you devoted a ton of time to the other factors elsewhere in the book. You seemed to end up with a pretty “big tent” view of addiction, acknowledging that pretty much every theory has some truth and value, but none are exactly right. It’s hard to express this in any one chapter though, without constantly caveating yourself. How did you end up feeling about this process? Any general thoughts on how much context people should give to studies like these, where the general premise is probably broadly true, but some of the specifics have questions?
Tim: After reading some of the critiques of this study, I considered taking it out. But then I got annoyed by some of the critics who claimed that the study had NEVER been replicated when it was actually mixed results from replications.
I read Alexander’s book, The Globalization of Addiction, and felt comfortable that there is a pretty wide body of research establishing significant environmental effects when it comes to addiction. And, in the popular press and general cultural understanding of addiction, I still think these factors are not well understood or well known.
This is why I included the study about returning Vietnam service members and indigenous populations. Different scientists, different approaches but affirming the same general points.
I did have another paragraph providing a caveat about the role of poverty and that if wealth were all you needed then you’d never see the same celebrity on MTV Cribs and in the tabloids going off to rehab. But there was a longer section there that didn’t make the cut.
The best framework isn’t connecting poverty and addiction but stress and addiction. Poverty is just one of the highly stressful experiences common in our world. But so was serving in Vietnam and, while I have no first-hand experience, so is being a celebrity.
Another interesting area of inquiry is that there is good reason to believe that intermittent access to resources is actually more stressful than a consistent lack of resources. Our bodies respond poorly to highly fluctuating environments. That area of research could have been a whole chapter on its own. The one other area I touch on it is my chapter on the “body” where I look briefly at genetic/epigenetic factors related to addiction.
Yeah, those are good points. The idea that stress and environment can play a roll in addiction seems pretty clear, though even your own story shows that can be complicated. You got addicted due mostly to large quantities of pain medication prescribed for a real need, but the tumultousness of your life at the time can’t have helped. For any critique of this study, even Scott Alexendar ended up saying the idea that ultimately unhappy people probably do more drugs than happy people seemed to be relatively self evident. So I think there’s something to this, though clearly it’s not the whole story. Addiction is not something that happens in a vacuum, even if there’s more going on. As they say, genetics loads the gun, environment pulls the trigger.
Alright, so that’s it for this week! Come back next week for our final post, and in the meantime enjoy this picture of me holding the actual book my brother signed for me! GETTING EXCITED!!!!